Frequently Asked Questions and Answers
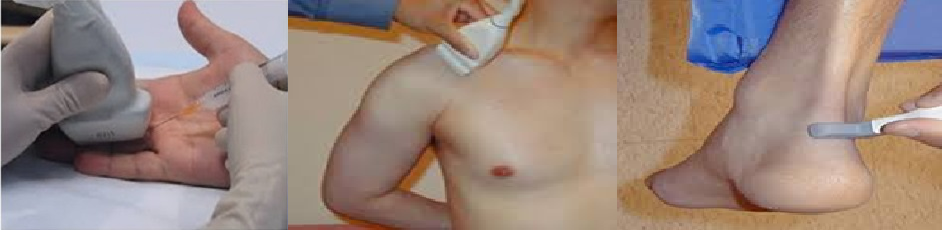
Ultrasound is safe and painless, and produces pictures of the inside of the body using sound waves. Ultrasound imaging, also called ultrasound scanning or Sonography, involves the use of a small transducer (probe) and ultrasound gel placed directly on the skin. High-frequency sound waves are transmitted from the probe through the gel into the body. The transducer collects the sounds that bounce back and a computer then uses those sound waves to create an image. Ultrasound images of the musculoskeletal system provide pictures of joints muscles, tendons, ligaments, and soft tissue throughout the body.
Ultrasound is widely available, easy-to-use and less expensive than other imaging methods.
Ultrasound imaging is extremely safe and does not use any ionizing radiation.
Ultrasound scanning gives a clear picture of soft tissues that do not show up well on x-ray images.
Ultrasound provides real-time imaging, making it a good tool for guiding minimally invasive procedures such as needle biopsies and fluid aspiration.
Patients with cardiac pacemakers and certain types of metallic implants in the body cannot safely undergo MRI however; can safely receive ultrasound imaging.
Ultrasound is also an excellent alternative to MRI for claustrophobic patients.
Compared to MRI, ultrasound may provide greater internal detail when assessing soft tissue structures such as tendons and nerves.
Because ultrasound images are captured in real time, they can show the movement of a soft tissue structure such as a tendon, joint or an extremity.
Ultrasound imaging is faster than MRI and does not require the patient to remain completely still, allowing infants to be imaged without sedation.
For standard diagnostic ultrasound, there are no known harmful effects on humans.
Ultrasound has difficulty penetrating bone and, therefore, can only see the outer surface of bony structures and not what lies within (except in infants who have more cartilage in their skeletons than older children or adults). For visualizing internal structure of bones or certain joints, other imaging modalities such as MRI are typically used.
Joint and soft tissue changes in Rheumatoid arthritis and other inflammatory arthritis including early diagnosis, disease activity and response to treatment.
Inflammation or fluid (effusions) within the joints and bursae.
Nerve entrapments such as carpal tunnel syndrome.
Tendon pathology like tenosynovitis, Tendon tears or tendinitis.
Muscle tears, masses or fluid collections.
Ligament sprains or tears.
Benign and malignant soft tissue tumors.
Ganglion cysts.
Hernias.
Foreign bodies in the soft tissues (such as splinters or glass).
General queries
The results of the scan will help your doctor to make a diagnosis and or plan treatment for you.
Musculoskeletal ultrasound examination is usually completed within 15 to 30 minutes but may occasionally take longer.
No. There is no preparation required for this examination.
During the examination:
You should wear comfortable, loose-fitting clothing for your ultrasound exam.
You may need to remove jewelry in the area to be examined.
You may be asked to wear a gown during the procedure.
For certain ultrasound examinations of the musculoskeletal system,
you may be seated on an examination table or a swivel chair. For other
ultrasound exams, you will be positioned lying face-up or face-down on
an examination table. The radiologist or sonographer may ask you to
move the extremity being examined or may move it for you to evaluate
the anatomy and function of the joint, muscle, ligament or tendon.
A warm gel will be spread on the area that is to be examined and a
small hand instrument (a transducer or probe) will then be moved
over the area.
Images form on a screen for analysis. You will not hear or feel the
sound waves. However, if you are feeling uncomfortable you can
tell your doctor.
Once the imaging is complete, the clear ultrasound gel will be wiped
off your skin. Any portions that are not wiped off will dry to a powder.
The ultrasound gel does not stain or discolor clothing
Ultrasound examinations are painless and easily tolerated by most patients. When the examination is complete, you may be asked to dress and wait while the ultrasound images are reviewed. After an ultrasound examination, you should be able to resume your normal activities immediately. A report will be sent to the referring clinician. The radiologist will also discuss with your clinician in case there is any unusual incidental finding requiring extended examination or urgent attention. Follow-up examinations may be necessary, and your doctor will explain the exact reason why another exam is requested.
Information for patients who have been referred for an ultrasound guided injection by the clinician.
Steroid injections are used to reduce pain and swelling. The injection may be given into a painful joint and may also be used to treat soft tissue inflammation such as tendons, bursae, plantar fasciitis, tennis elbow etc.
The injection will be performed by a radiologist experienced
in musculoskeletal interventions.
Consent
The procedure will be explained to you and you can ask
any question you like to before the procedure.
Procedure
The radiologist will first perform a quick ultrasound
examination to indentify the parts where injection has to
be given. The patient is made comfortable in either lying or
sitting position. The skin is cleaned with a sterile solution
and a local anesthetic may be used prior to injection to
reduce pain.
It is possible that you may get more than one injection or the
part to be injected modified after ultrasound examination
depending upon the findings, e.g. in a swollen ankle, tenosynovitis
may be the main reason instead of ankle joint synovitis.
The radiologist will discuss the same with the referring clinician.
After the Injection
The injected area may feel uncomfortable and once the anesthetic
wears of you may feel pain for some time.
You are advised to rest the injected joint /part for one day.
You can start doing your usual activities after a day.
Things to know
The purpose of steroid injection is to reduce pain and inflammation
in the effected joint or tendon injected.
Inform your doctor if you notice redness or swelling around the area
injected or a high temperature and also if you develop any
allergy e.g. skin rashes
Alternatives
Your doctor would have already discussed with you about other options
like increasing systemic treatment. Surgery is another possibility but
it is often advised when conservative measures fail.
Write to us
Have a Question? Simply send us a message. We'll give you the perfect answers.

